Senators to grill Moderna CEO on its four-fold price hike of COVID-19 vaccine that feds helped make
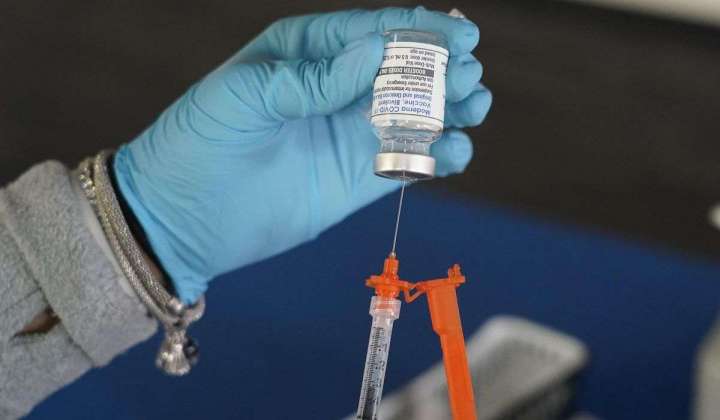
Prominent drugmakers want to more than quadruple the price of their COVID-19 vaccines when the shots transition to the commercial market later this year, sparking a showdown with congressional lawmakers who say Pfizer and Moderna benefited from taxpayer largesse and are now gouging the public to pad handsome profits.
Senate Health Committee Chairman Bernard Sanders will grill Moderna CEO Stéphane Bancel over the proposed hike at a highly anticipated hearing next week that will underscore tensions between Big Pharma and lawmakers outraged over ballooning drug prices.
Mr. Sanders, a democratic socialist from Vermont, is angry because Moderna benefited from collaboration with the federal government to bring the COVID-19 vaccine to market but is now planning to charge $110 to $130 per dose once federally purchased stockpiles are used up — a steep increase from the $15 to $26 it charged the government earlier in the pandemic.
Mr. Sanders says it costs $2.85 to make each dose or 2.2% of what Moderna plans to charge.
The transition to the commercial market will likely coincide with a fall booster campaign that uses new shots against circulating strains.
Drugmakers will be under pressure to fulfill their pledges that no American will have to reach into their pocket for COVID-19 shots. The companies say patient-assistance programs will help the uninsured, a move lawmakers hailed as a step in the right direction while fretting the programs will be insufficient or inundate people with paperwork.
Lawmakers also want to know how much the companies will charge private insurers and government programs after rebates and discounts are factored in.
“The huge increase in price will have a significantly negative impact on the budgets of Medicaid, Medicare and other government programs that will continue covering the vaccine without cost-sharing for patients,” Mr. Sanders told The Washington Times. “It’s not a coincidence Moderna announced plans to give free vaccines to the uninsured after we invited them to testify.”
The standoff between lawmakers and drugmakers underscores the thorny transition from a COVID-19 response that relies on direct federal intervention to one in which the virus is treated like other diseases in the complex and costly U.S. health care market. It also speaks to a long-running concern: That drugmakers make huge profits from government-sponsored research but don’t return the favor.
“They ought to be obligated to put a share of windfall profits back into the NIH research budget. A hearing is fine but Congress needs to act to prevent this sort of exploitation of the taxpayer, who pays for research that companies sell back to them at high prices,” said Arthur Caplan, director of the division of medical ethics at the New York University Grossman School of Medicine.
Lawmakers in recent years have dragged executives to Capitol Hill to testify about costly drugs for diseases like Hepatitis C. President Biden is browbeating insulin companies to cap out-of-pocket costs for diabetes sufferers at $35 per month after Democrats’ attempts for widespread limits ran into GOP opposition last year.
Pfizer landed on Congress’s radar in October when the drugmaker told investors that a potential U.S. list price between $110 and $130 per single dose vial “reflects the value of the vaccine and as well the thresholds for what would be considered a highly cost-effective vaccine.”
Moderna then floated a similar price increase.
Senate Democrats were livid, pointing in scathing letters to the nearly $10 billion the Massachusetts company received in federal government funding to boost its manufacturing capacity, execute large-scale clinical trials and secure doses. They said Moderna reported $12 billion in net income for 2021.
“Your company has already earned billions in profits from the vaccine, which benefited from extensive taxpayer support for research and development, and your proposed price increase threatens to reduce access to a life-saving vaccine while boosting your company’s profits,” Sens. Elizabeth Warren of Massachusetts and Peter Welch of Vermont wrote to the company in January.
The Kaiser Family Foundation says the proposed commercial prices would be far above the roughly $15 that Moderna charged the government for its first tranche of shots in mid-2020, or the $26 it sought for the updated “bivalent” booster shots that attack both the original strain of the virus and omicron variants.
KFF analysts said the cost of vaccinating just half of Americans under the proposed commercial prices would exceed the cost of purchasing enough vaccines for everyone in the country at the federal bivalent-booster price. Even so, they noted that even at higher spending levels driven by commercial pricing, COVID-19 vaccination is likely to be cost-effective compared to not vaccinating, given the economic benefit of preventing hospitalizations and deaths.
Lawmakers are pressuring Moderna in part because its scientists worked alongside government teams at the National Institute of Allergy and Infectious Diseases during the rush to combat the coronavirus in 2020. Moderna’s shots became a dominant option alongside the ones that Pfizer developed with its German partner, BioNTech.
Federal data shows over 250 million doses of the Moderna versions have been administered in the U.S. alone.
The two-dose primary vaccines and booster shots use groundbreaking messenger RNA technology, which injects a snippet of genetic code — encased in a bubble of fat — to instruct the body on how to recognize and combat the virus.
Government news releases on the effort typically noted the shots were “co-developed” by the NIAID and Moderna. The effort included a dramatic weekend in January 2020 in which NIAID and Moderna scientists worked to figure out the genetic sequence needed to mimic the virus’s spike protein.
Moderna earlier this year made a $400 million “catch-up payment” to NIAID, which will be shared with two academic institutions, for royalty rights related to a molecular technique it borrowed from the agency in making the vaccine.
However, Mr. Bancel recently pushed back on the idea the government created the platform for its vaccine.
“What the government did — and we’re very grateful for it and I think they got a lot of value out of it — is to accelerate the development of a vaccine. We would have funded the vaccine, it would just have taken longer,” he said during a Wall Street Journal Health Forum this month.
Responding to congressional criticism, the company said the government-funded its clinical trials “to enable the scale and speed it wanted.” Moderna also said it discounted the price of its vaccine early on to reflect public contributions.
Also, the company said it spent $1.4 billion in private funding to open its Norwood, Massachusetts, manufacturing facility in the summer of 2018, well before the COVID-19 pandemic.
The Department of Health and Human Services says the transition to the commercial market will likely occur in the fall for vaccines and at the end of the year for treatments like Paxlovid. In a recent blog post, a top HHS official pressured drugmakers to keep costs in check.
“We fully expect that industry will look to the example that the U.S. government has set by pricing these products at a reasonable rate and eliminating access hurdles for every American. Additionally, we expect that insurers will keep any out-of-pocket costs, including co-pays and deductibles, as low as possible for consumers,” Dawn O’Connell, assistant secretary for preparedness and response.
In a statement on its pricing decisions and congressional scrutiny, Pfizer stressed the fact it relied on its investments to develop the vaccine on its own.
“Pfizer did not receive any government funding for the development of the Comirnaty COVID-19 vaccine or Paxlovid. The funds received by Pfizer from the U.S. government were payments for products that the government acquired, but only upon delivery of the products,” the company said in a statement. “We have invested from our own resources at risk and are prepared to continue to bear the costs of development and manufacturing to advance COVID vaccines and therapeutics.”
Moderna, meanwhile, said its vaccine reflects “the value of our vaccine from both a human health and economic perspective.”
“Our vaccines have helped protect the lives of millions of people around the world and have allowed both the U.S. economy and economies around the world get back to work,” company spokesman Christopher Ridley said. “Our vaccine will be priced similar to other vaccines, including those for hepatitis and pneumonia. These vaccines are all part of preventative patient care and are priced to reflect the value they provide to society in avoiding healthcare and economic costs associated with disease, like costly hospitalizations.”
Jennifer Kates, a senior vice president at the Kaiser Family Foundation, said a range of factors can impact what drugmakers decide to charge, including manufacturing costs and whether demand for the drug is rising or decreasing.
It is “sort of a market assessment, what will the market bear for this?” she said. “That’s different from the government coming in and saying, ‘We want millions of doses and here’s what we’re going to pay.’”
Demand for COVID-19 vaccines is dwindling. Uptake hit a high point in April 2021 during the early rush to immunize the population, with over 3 million shots entering arms per day. Average delivery has fluctuated with various booster campaigns since then but generally dwindled, reaching around 1.8 million shots per day during the fall 2021 booster drive and an average of 650,000 shots per day during the pre-winter booster drive in October last year.
More than eight in 10 Americans have received at least one dose of a COVID-19 vaccine, while over two-thirds of the population has completed a two-dose series.
Yet even as federal regulators outline plans for boosters, demand for the extra shots has dwindled. Only 16% of the U.S. population received one of the bivalent boosters, which were unveiled last fall as part of a push to match the shots to circulating strains.
Demand for the bivalent boosters, specifically, averaged 600,000 doses per day in October, or shortly after their authorization. That average had fallen to around 41,000 shots per day by the start of this month, according to the Centers for Disease Control and Prevention.
“The only reason we purchased them [in 2020] was because we felt demand would exceed supply and we wanted distribution to be equitable and get to the neediest first,” said Paul Mango, a former top official at the Department of Health and Human Services. “Supply has now exceeded demand for quite a while.”
Mr. Mango said the Trump administration determined that vaccine makers’ costs were “down closer” to what the government paid for doses in 2020, so the proposed commercial price “sounds like one helluva profit margin.”
While vaccine makers may forfeit certain liability protections once Mr. Biden unwinds COVID-19 emergency protocols in May, that would not entirely explain the difference, he said.
Mr. Mango also noted that Moderna charged the government less than Pfizer in early rounds of purchasing, essentially accounting for the government’s upfront assistance.
“Congress should not interfere with the free market at this point but government officials should be free to point out that they believe the manufacturers are charging exorbitant prices if they choose,” Mr. Mango said. “Freedom is bilateral.”
The average person won’t see a direct cost when they get the vaccines under commercial prices, particularly if they are covered by government-run or private insurance, though the higher costs must be absorbed by the system.
“From our assessment, from looking at private insurers’ filings, it potentially could have an effect on premiums,” Ms. Kates said.
She said a parallel issue is whether the patient-assistance programs will be adequate or cover everyone who wants the vaccine.
Pfizer said health professionals who want to vaccinate an uninsured patient should contact the Pfizer Patient Assistance Program to understand the eligibility requirements. Eligible patients will not be expected to pay upfront, though clinicians and pharmacies will need to have to submit documentation to receive reimbursement.
Moderna said its free drug program will provide COVID-19 vaccines “at no cost – the details will be determined before our vaccines enter the commercial market.”
Health experts said senators can press Moderna for the details of its program but will not be able to impact the list price of the vaccine.
At this point, all they can do is huff and puff.
Moderna got “enormous government support, NIH owns some of the patents on mRNA technology, they’ve gotten money through Operation Warp Speed, they got pre-purchase agreements from the government that were lucrative. I think they’re acting entirely irresponsibly to make it so unaffordable,” said Lawrence Gostin, a global health law professor at Georgetown University. “Having said that, I think all the hearings can do is blame and shame them, reprimand them for being bad citizens. Unless Congress actually passes legislation, signed by the president — which is almost inconceivable at this point — Moderna can do what it wants as a private company.”
For more information, visit The Washington Times COVID-19 resource page.






